Microvascular Free Flap Reconstruction for Diabetic Foot Ulcers: A Limb Salvage Approach
Introduction
The lifetime risk of developing a foot ulcer in patients with diabetes can be as high as 15%25%. Diabetic foot ulcers result from a combination of peripheral neuropathy, infection, and ischemia. With specialist multidisciplinary care, approximately two-thirds of patients who develop a diabetic foot ulcer will eventually heal. However, one-third of patients’ wounds fail to heal, placing them at high risk of amputation. Diabetic patients account for 40%–70% of all lower-limb major amputations. Studies have shown that the five-year mortality rate following a major amputation in diabetic patients is significant and exceeds that of many major cancers. Patients with large tissue defects, deep space infections, osteomyelitis, or exposed tendon or bone may require microvascular free tissue transfer to heal their wounds and salvage the limb. Although successful limb salvage using free flaps has been demonstrated, their use in diabetic foot ulcers has been less well documented, often being concentrated in highly specialized units. It is estimated that 2%–25% of diabetics with large tissue defects would benefit from microvascular free flaps. Improved survival after successful limb salvage using microvascular free flap transfer has also been reported.
Case Report
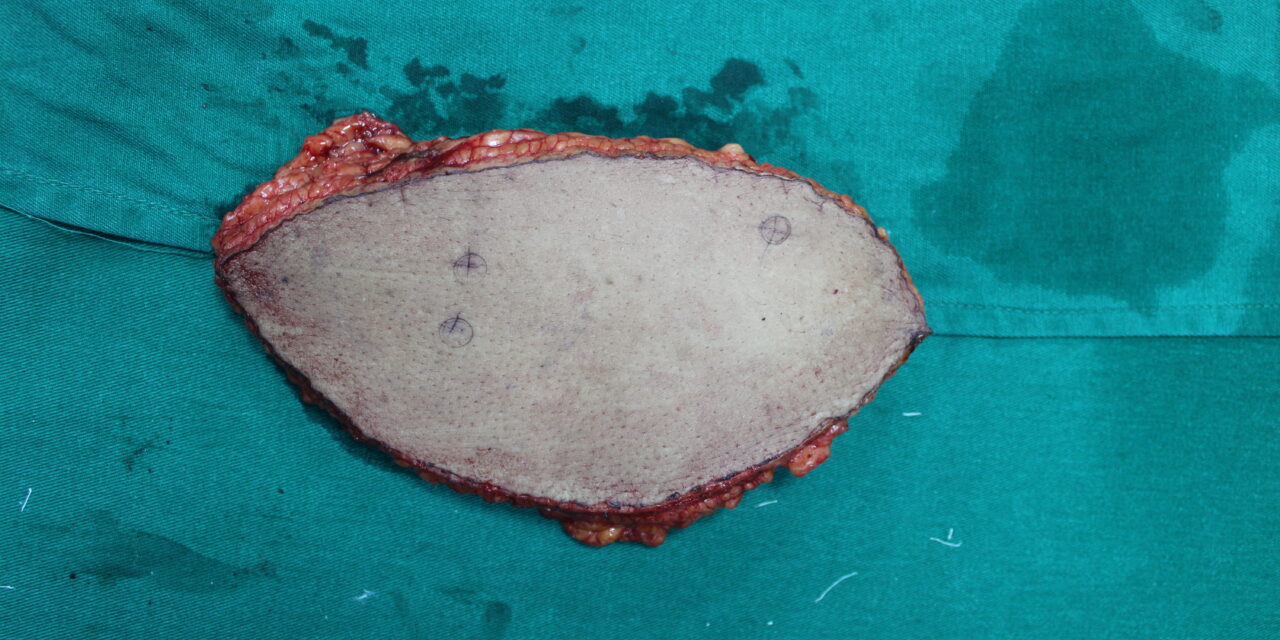
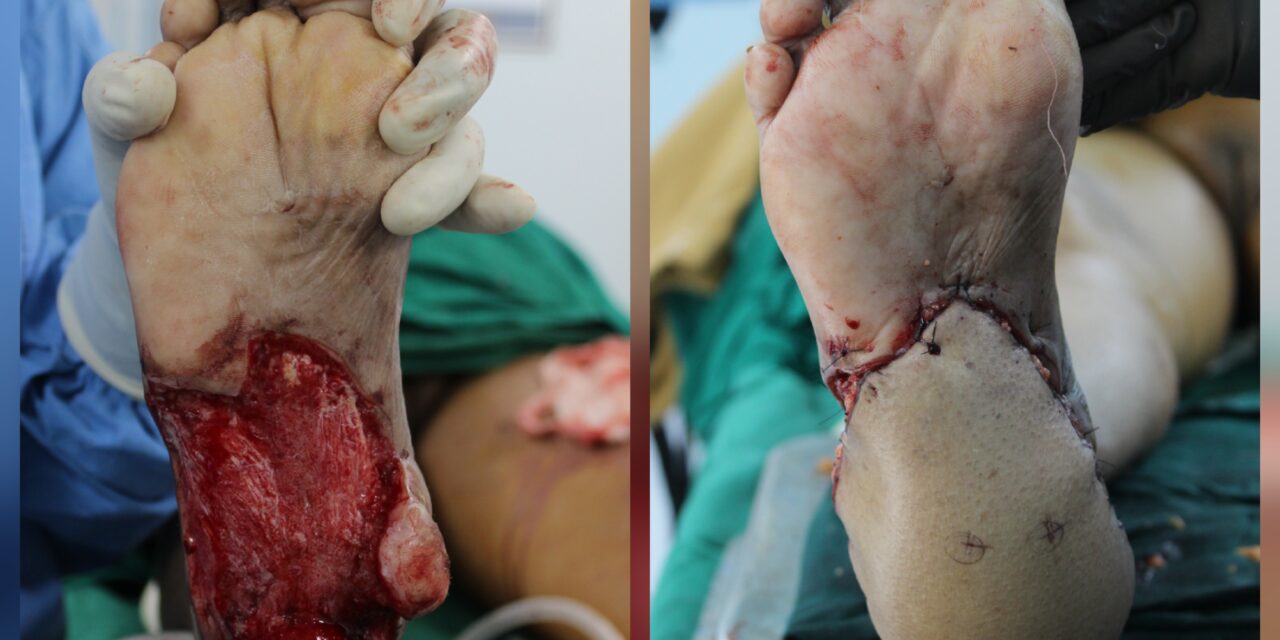
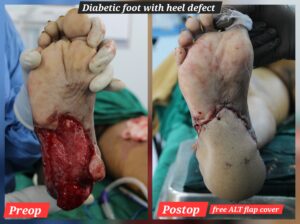
A 56-year-old female with type 2 diabetes and hypertension, controlled with oral medications, presented to the General Surgery Department with a history of a diabetic foot ulcer o”er the heel, complicated by spreading cellulitis. The wound was surgically debrided, leaving a large defect measuring approximately 15 x 10 cm, exposing the tendoachilles and calcaneus bone. An arterial Doppler study revealed atherosclerotic changes with monophasic flow in both the peroneal and posterior tibial arteries (PTA). The foot was being perfused only by the anterior tibial artery (ATA). A below-knee amputation was initially planned. However, a referral was made to the Plastic Surgery Department to explore the possibility of limb salvage using a microvascular free flap. The patient was counseled about the potential benefits and risks. Given the compromised blood flow in the ATA, using it for flap anastomosis might have compromised the residual foot blood supply. Therefore, the decision was made to anastomose the flap to the proximal healthy PTA using a vein graft. The procedure was successfully performed by Dr. Nagamallesh C.S, Plastic Surgeon, with the assistance of Dr. Prajwal Shastry and Dr. Gaganadeepa. C, Under the guidance of Dr. K S Gangadhara, Dr. Krishnamurthy, and Dr. Vijay BN, with the support of Department of Anesthesiology headed by Dr. Renuka. The patient’s limb was successfully salvaged with microvascular reconstruction. Postoperatively, the patient recovered well and is now independently ambulatory, without significant psychological trauma.
Conclusion
This case highlights the importance of a multidisciplinary approach in managing complex diabetic foot ulcers. Microvascular free flap reconstruction can be a limb-saving procedure, even in patients with severely compromised arterial flow, when carefully planned and executed. Early referral to specialized units can offer patients with otherwise unsalvageable limbs a chance for functional recovery and improved quality of life.